How your brain can heal itself
Groundbreaking research offers new hope for people with chronic pain, multiple sclerosis and more
Madeline A. Lancaster / IMBA
Share

A South African man with Parkinson’s disease, a degenerative disorder that often leaves its sufferers immobile, walks his symptoms into submission. A Broadway singer, silenced for 30 years by multiple sclerosis, recovers his voice. And in California, a psychiatrist and pain specialist rids himself of 13 years of chronic pain within a year, without drugs or surgery, through his brain’s own efforts. Those individuals, and thousands like them, achieved those results, writes Norman Doidge, a Toronto psychiatrist and author of The Brain’s Way of Healing, precisely because the human brain is a generalist par excellence. The prevailing 20th-century view was that it was too specialized for its own good—a fixed machine made up of discrete parts that can break down, never to function again. That concept no longer stands up to scrutiny.
The brain is actually a supple, malleable organ, as ready to unlearn as it is to learn, capable of transforming vicious circles into virtuous circles, of resetting and repairing its internal communications. Far more than once dreamed possible, the brain can—if not always cure—heal itself.
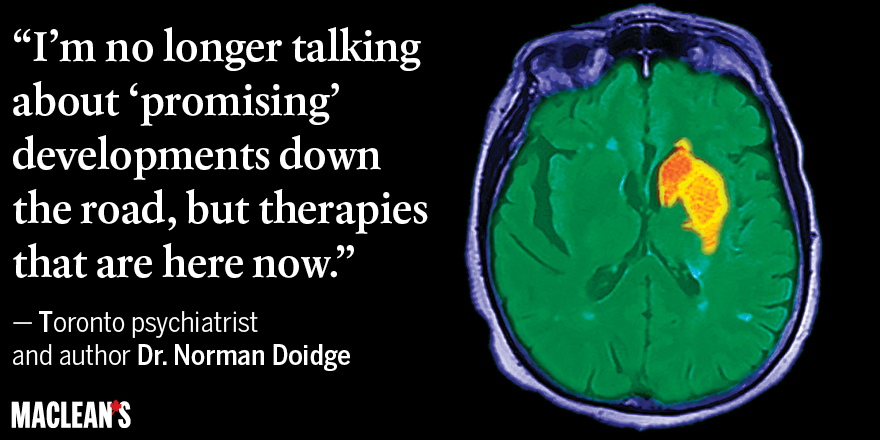
Doidge wrote about the brain’s remarkable ability to recalibrate itself—what doctors call neuroplasticity—in his 2007 bestseller The Brain That Changes Itself. His new book recounts an astounding array of radical improvements in brain problems long thought irreversible. There are newly effective therapies, leading to improvement in, and sometimes even complete cures, for conditions ranging from stroke to traumatic brain injuries, learning disorders and missing brain parts. Even Parkinson’s and MS symptoms can be improved in new ways. “Like Marshall McLuhan said, the future is already here,” says Doidge in an interview. “The early neuroplasticians had to battle to get their findings accepted but now the field is not remotely controversial. I’m no longer talking about ‘promising’ developments down the road, but therapies that are here now. Patients and their caregivers just have to know who is doing things they thought impossible.”
And, crucially, to work hard at their own care. “We have been habituated to a way of thinking,” notes Doidge, which derives from what he calls the military metaphor of medicine, “the idea that the patient is merely the passive battleground where the two antagonists, the doctor and the disease, fight it out. The patient’s job is to endure until the doctor comes up with something, or, these days, to become involved in a fundraising event that will send money to researchers so they or the drug companies can come up with the answer.” But the plastic brain, capable of so much, still needs the help of mind and body to realize its possibilities.
Consider Dr. Michael Moskowitz, who knows pain both professionally and intimately. The co-operator of Bay Area Medical Associates in Sausalito, Calif., Moskowitz is a star in the treatment of pain, the man who sets the exams in pain medicine for aspiring American doctors. His clinic treats intractable cases, patients who have tried everything for their agony—all known drugs, nerve blocks, acupuncture—without result. “We are where people come to die with their pain,” he told Doidge. By 2007, 13 years after a waterskiing accident, it looked like Moskowitz would be one of them. The acute pain from his neck injury had morphed into permanent, and growing, chronic pain.
It did so via the same mechanisms that create that transformation in anyone. “Chronic pain is plasticity gone wild,” Doidge says. The injury to Moskowitz’s neck had also affected his body’s pain system, specifically the neurons in the brain associated with the neck area, causing them to fire repeated false alarms long after the neck had healed. What happened next illustrates core laws of neuroplasticity. Neurons that fire together, wire together: the more Moskowitz’s pain signals flared, the better and quicker they became at it. Use it or lose it: the fight for brain territory is competitive. The more Moskowitz favoured his neck because of the pain, the less the neurons involved with it had to do, and the more vulnerable they become to hijacking by nearby areas, including the pain sensors now working overtime. Moskowitz was caught in a vicious circle. His pain, 3/10 on the standard scale at the best of times, and spiking frequently to 8/10, was only getting worse. “Plasticity is a blessing when you’re listening to classical music and developing an appreciation for it,” Doidge wryly notes, “but it’s a curse when you are reinforcing pain.”
As his quality of life inexorably eroded, Moskowitz sat down to read 15,000 pages of cutting-edge neurological research, seeking a way to make plasticity work for him. Moskowitz concentrated on two areas of the brain among the dozen that do at least some pain processing, the posterior cingulate and the posterior parietal lobe, areas whose primary purpose is to deal with visual information.
He knew already that when a brain area is processing pain it uses about five per cent of the neurons in the area, but the reinforcement involved in chronic pain means about 15 to 20 per cent of the neurons become involved. By concentrating on an image of his brain—an image in which it changed from being lit up by pain activity to being calm and pain-free—Moskowitz thought he could quiet the original pain receptors and force the hijacked neurons back to their day jobs as visual processors.
It required relentless dedication at first, a conscious response to every twinge. In three weeks, Moskowitz thought he detected slight improvement, enough to spur him on; by six weeks the pain that had spread to his back was gone; within a year he was almost always pain-free everywhere. He had turned the vicious circle virtuous. “Relentlessness was the most important factor, absolutely,” Doidge agrees. “As a psychiatrist, I know that if you reframe a symptom attack as an opportunity, if instead of becoming crestfallen and pulling back, you treat every pain, anxiety or inhibition—reframe it as your moment—that’s the route to altering that circuitry. That’s what Moskowitz did. He didn’t let a single twinge of pain go by.”
Intense dedication is a hallmark of those who, all on their own, accomplish large-scale change in their brains. John Pepper, a South African now in his late seventies, was diagnosed in his thirties with the incurable, chronic, progressive neurodegenerative disease known as Parkinson’s. By all odds he should be immobile, if not dead, by now, but Pepper has fought his symptoms to a standstill by vigorous exercise carried out with ferocious determination and conscientious attention to detail. “Even as his unconscious ability to walk unravelled,” Doidge explains, “Pepper realized that if he analyzed how he walked and used his conscious mind to guide him, he could still do it. So he used a different part of his brain, the frontal lobes, and—like a child learning to walk—thought himself into efficient walking.”
Pepper’s case has fascinated everyone who has encountered it, partly because of his admirable bloody-mindedness, and partly for the way it demonstrates the importance, in recalibrating brain activity, of walking, the king of exercise. “It’s our evolutionary history at work,” Doidge argues. “When do animals do a lot a walking? When the environment they are in is being swarmed by predators or falls short of food. Moving to a new territory means entering a place where they have to do a lot of learning. When the brain takes note of a lot of walking, it and the body together secrete growth factors which put the brain into a super-plastic state, primed to learn.”
People with Parkinson’s have six times the dementia rate of those who do not, and Pepper is reaching what are the danger years for anyone, yet his mind is sharp. That, together with his mode of exercise and the first-the-right-heel-then-the-left-knee precision with which he pursues it, raise a question about Alzheimer’s, a disease where both exercise and conscientiousness are proven factors in delaying onset. Is Alzheimer’s a disease of plasticity, or rather of its absence? Doidge is cautious in response. “There are so many ways of looking at Alzheimer’s. Most researchers analyze it chemically, because of the proteins involved, in hopes of finding alleviating drugs, but to look at Alzheimer’s that way is to put it under the microscope at very high power—it is more holistic to think of an Alzheimer’s brain as one that is losing plasticity.”
Whether walking battles the onset of dementia through its link to plasticity or by its more general health benefits, it’s one of the most potent anti-dementia forces known. “Now we have the Cardiff study looking at the British men over 30 years and it shows that if you did five things, including walking at least three kilometres a day,” Doidge says, “the risk of dementia falls a staggering 60 per cent. If any medication did that, it would be the most talked-about drug in history.”
Not that drugs have any role in the story Doidge tells. Moskowitz, who has switched the goal of his clinic from pain management to pain eradication, recognizes that he himself (and the likes of Pepper) is an outlier set apart by his iron determination. Not all his patients can follow him down his own relentless road. Even so, Moskowitz does not always seek to aid them with drug therapy—instead devoting considerable effort to weaning them from painkillers—but with touch, sound and vibration. It’s a pattern Doidge sees everywhere. “Almost all the success stories involve a combination of mind and energy.”
Much of The Brain’s Way of Healing is devoted to non-invasive energy therapies. The author is particularly enamoured with light therapy, once far more prominent in Western medicine than it is now. Doidge likes to quote Florence Nightingale, who said “Light is not only a painter but a sculptor,” after she took note that wounded soldiers in outdoor field hospitals in Crimea recovered better than those stuck indoors. “We are far more transparent than we think and more sensitive to light than we think. So I have an entire chapter on the use of light, including cold lasers, to heal the brain.”
Light and other energy therapies have fallen from favour, Doidge believes, because for 50 years scientists have focused on the brain’s material and chemical side. Chemicals do work in small regions for signalling, he says, but the true universal language of the brain lies in its pattern of electrical signals. “All our senses take energy from outside and translate it into another form of energy inside the brain. Clinicians can now use these natural forms of energy to ‘talk’ to the brain.” And nothing speaks more loudly and clearly than the electrical pulses of the PoNS.
Originally thought of by its inventors as an aid for brain-injured people with balance troubles, the Portable Neuromodulation Stimulator has astonished even them with its effectiveness over a range of conditions and, especially, the speed with which it helps. (See the book excerpt that follows.) A small, pocket-sized device, part of which went into the mouth and rested on the tongue and part of which stayed outside—144 electrodes that fired off electric pulses to activate the tongue’s sensory neurons. After two weeks of sessions with it, a voiceless MS patient could sing; a woman immobilized by Parkinson’s could walk; a stroke victim who couldn’t understand a newspaper article could read whatever she wanted.
All this because the tongue, Doidge says, “is the royal road to the brain”—with no dead skin and a moist surface making it an excellent conductor, and rich in sensory preceptors for touch, taste and pain that lead directly to the brain stem. “The PoNS turned out to be a very good stimulator for the whole brain.” Doidge thinks it clears up “noise” in the brain caused by disease or injury. “People tend to think neurons are either dead or alive afterwards, but actually many are firing at an irregular or wrong rate. Incoming information is thus chaotic and noise-filled, with even the healthy cells unable to communicate.” The PoNs, via the tongue’s access to the brain stem and hence the entire brain, can reset the circuitry, allow effective electrical communication and return the brain to a state of equilibrium. That’s why the application is so wide-ranging: with the noise gone, the brain starts working with what it has, in whatever condition it finds itself.
For decades, Doidge remarks, scientists wouldn’t use “healing” and “brain” in the same sentence, because they thought the brain was so sophisticated that it lacked self-healing powers. That turned out to be wrong—the brain is even more sophisticated than anyone realized.
EXCLUSIVE EXCERPT:
First he noticed it was becoming hard to sing, a nightmare because that was how he made his living and singing was who he was. Then he could barely sing at all but could still speak his lines. And then over a couple of years he began to lose his speaking voice, until it became wispy thin and trailed off, so that he could generate only short, barely audible bursts of whispered air.
“It was agonizing to watch him lose his beautiful singing voice, heartbreaking. I fell in love with that voice,” said Patsy Husmann, his wife of 50 years. Ron Husmann was a singer of first rank on Broadway, on television, and in film, and throughout the 1960s and 1970s his deep baritone was everywhere. He sang in Camelot opposite Robert Goulet. He co-starred in The Gershwin Years with Frank Sinatra, Ethel Merman and Maurice Chevalier. He starred on Broadway in Tenderloin, and worked with the leading ladies Debbie Reynolds, Julie London, Bernadette Peters and Juliet Prowse in more than half a dozen other Broadway shows. He toured as the lead in Irma La Douce, Show Boat, South Pacific, and Oklahoma! Singing live, in a theatre that held 3,000 people, Ron could be heard by everyone without using a microphone, while the rest of the cast required one.
The bass register begins to mature in richness only in a singer’s thirties, and completely fills out in his forties. Ron was at his peak at 44 when, as he whispered, “it stopped dead.”
As with many people who are eventually diagnosed with multiple sclerosis (MS), it took doctors a number of years—nine, in his case—to realize that his lost voice and a complicated package of other symptoms were caused by MS. In MS, one’s immune system, instead of attacking invading organisms as it should, turns against the brain and spinal cord and attacks the fatty sheath around the long projections of the nerves. This sheath, called myelin, functions as insulation and can increase the speed of the conduction of a nerve signal 15 to 300 times.
Because antibodies can attack myelin almost anywhere in the brain or spinal cord, each patient gets a different version of MS, and each person’s symptoms unfold in a different way. Ron’s deep voice was stripped of its beauty in a series of onslaughts. First the middle tones began to disappear; then suddenly he didn’t have the low notes, for which he was most famous. He went to all the “voice people” who serve performing artists. Onstage, directors had to mike him up so he could be heard, until there was nothing much left to amplify. By the time his singing career was ruined, he was able to hit only about eight notes around middle C.
As the muscles of his legs and arms wasted away, he needed to walk with a cane; then he needed two canes, the kind that go all the way up the arm; then he sometimes had to use an electric cart and gained 50 lb. from lack of exercise. Next he began to have trouble with balance. Standing with his eyes closed, he couldn’t keep himself erect. He had trouble swallowing—always a terrifying symptom. He was increasingly choking on his food because the brain stem, which coordinates the rhythmic contractions of the throat muscles, was no longer working properly. His worst symptom was his unrelenting exhaustion. He got to the point where he could only whisper into the phone for perhaps a minute, until his voice broke up so badly that he imagined he would have to stop trying to whisper altogether.
By coincidence, perhaps, a friend of Ron’s from high school also developed MS and voice problems. Now a retired professor living in Madison, the friend told Ron that a laboratory there, at the University of Wisconsin, had invented a strange device that you put in your mouth to help MS symptoms. The inventors were using the device to treat a range of MS symptoms, not only voice problems. Though it didn’t cure MS, if it was used regularly, it “reset” the brain, so it fired clearer signals and vastly improved its functioning. The lab had a strange name, the Tactile Communication and Neurorehabilitation Laboratory, and it was run by three men: Yuri Danilov, a Russian neuroscientist (and former Soviet soldier); Mitch Tyler, an American biomedical engineer (formerly of the U.S. Navy); and Kurt Kaczmarek, an electrical engineer.
The founder of the lab, Dr. Paul Bach‑y‑Rita, had recruited them. Bach‑y‑Rita, who had recently died, was a legendary figure, one of the first advocates of using brain plasticity in healing. A physician who worked as a neuroscientist, he was the first of his generation to argue that the brain is plastic from cradle to grave, and he used that understanding to develop devices that facilitated positive plastic change. Devices that he developed helped blind people see and helped restore balance lost after brain damage; they also included computer games for stroke patients to train their brains to restore lost functions.
When Ron arrived at the lab, he saw a small, modestly equipped room in an old building. It had a loading dock at its entrance, the hallway was under construction, and as one patient said, it “did not look like the home for scientific miracles.” Ron’s attitude was “This may work, this may not. What have I got to lose?” The team reviewed his medical records and did tests and recordings to determine his ability to walk and balance. They took him to the university’s voice assessment department and recorded his speech, which was incomprehensible, broken up, and appeared as little dots on the monitor. When the baseline testing was complete, they took out the device he had heard about.
It was small, fitting into a shirt pocket. It had a cloth strap attached, and some of the scientists in the lab wore it hanging around their necks, like a pendant. The part that went into the mouth and rested on the tongue looked like a wide stick of chewing gum. This flat part had 144 electrodes on its underside, which fired off electric pulses, in triplets, at frequencies designed to turn on as many of the tongue’s sensory neurons as possible, by generating a pattern of stimulation that roved across the underside of the device. This flat part was attached to a tiny electronics box, about the size of a matchbox, which sat outside the mouth and had some switches and lights on it. Yuri, Mitch, and Kurt called it the PoNS, named, tongue‑in‑cheek, for a part of the brain stem called the pons, one of the device’s main targets. The acronym PoNS stands for Portable Neuromodulation Stimulator, because when it stimulates the neuroplastic brain, it modifies and corrects how the neurons are firing.
The team asked Ron to put the device in his mouth, while he stood as straight as he could. It painlessly stimulated his tongue and its sensory receptors with waves of gentle signals. Sometimes the stimulation tingled, and sometimes it became barely noticeable, and when it did, the team would adjust the dial, turning it up. After a while, they asked him to close his eyes.
After two 20-minute sessions, Ron was able to hum a tune. After four, he was able to sing again. At the end of the week, he was belting out Old Man River.
What was most remarkable was that Ron’s improvement, after almost 30 years of steadily worsening symptoms, was so rapid. He still had MS, but now his brain circuits were functioning so much better. He stayed at the lab for two weeks, working Mondays through Fridays, practising with the device in his mouth, resting, and practising again. He did six sessions a day during the first week—four in the lab, two at home. Electronic voice testing showed huge improvement, a steady stream of sound. His other MS symptoms started to improve. The day he left, the man who had come in wobbling on a cane tap-danced for the team.
I spoke with Ron two months after he returned home to Los Angeles. He had brought the device home to practise with and reinforce his gains. Now that he had his voice back, he was gushing words—at times I had to ask him to talk more slowly, so I could get it all down.
“You can imagine if you haven’t sung for 28 years, what it’s like suddenly to sing again. The fact that I could carry a tune, and hook one note to another, after four 20-minute sessions, was astounding and emotional—more than emotional—I broke down. They told me to hum and vocalize while the thing was in my mouth. I gradually realized my voice was getting stronger. The next day Yuri said, ‘You don’t need that cane.’ That day I got rid of it. By the third day, I was able to stand without any support, and with my eyes closed. By the time I left, I could sing two octaves. I was a bass baritone, and I had a low E that I could sing in public, and when I did Annie Get Your Gun, I got up to an F sharp. And . . . I can be loud now! I was so loud in their lab, they had to put their fingers in their ears. And now when we walk our dog every night, I walk so fast my wife can hardly keep up with me.”
Then he said to me, “Do you realize that we have been talking for a full hour?”
“I wasn’t expecting you to sound younger than I do,” I said finally. “Your voice sounds like that of a man decades younger.”
He took a moment to think. “Well, maybe it should,” he laughed. “I haven’t used it for 30 years.”
From The Brain’s Way of Healing. Copyright © 2015 by NormanDoidge. Reprinted by permission of Penguin Random House. All rights reserved.