The coronavirus can’t be contained. Are you ready?
The chance to contain COVID-19 has passed. What will Canada do when it hits our cities, schools and hospitals?
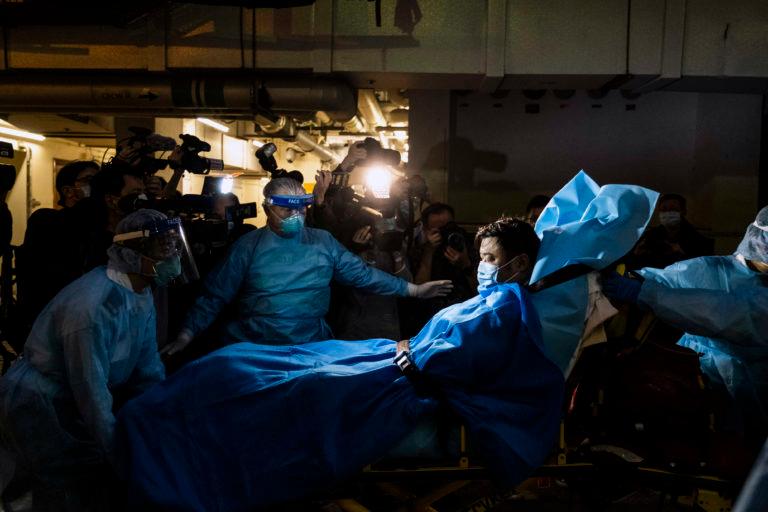
Paramedics transport a man believed to be Hong Kong’s first COVID-19 case, in January (Lam Yik Fei/The New York Times/Redux Pictures)
Share
Dr. Vanessa Allen received a text in late January from the medical director for infection prevention and control at Sunnybrook Hospital in Toronto. He needed to chat.
Allen is chief of medical microbiology at Public Health Ontario’s laboratory, which had recently started testing samples for the 2019 novel coronavirus, all of which had come back negative to that point. Jerome Leis at Sunnybrook was getting in touch because he had a case on its way that would likely be different.
A 56-year-old man had arrived at Sunnybrook that day with a fever and dry cough. The patient had just returned from a three-month visit to Wuhan, China, leaving two days before the Chinese government shut down the city’s buses, trains, ferries and airport. An X-ray of his lungs showed results consistent with a viral pneumonia.
The lab stayed open all night working on the specimen; they needed to be absolutely sure one way or the other. Fortunately, Chinese scientists had already determined the genetic code for the new coronavirus and shared the results internationally. “During SARS [in 2003], it took us more than four months to figure out what the virus was,” Allen says. “We didn’t have a test. We didn’t know who had it and who didn’t.”
Allen describes the test for the new coronavirus, known as COVID-19, as being akin to making photocopies of the genetic code in the patient’s sample, and amplifying it to see if it matches the genetic code of the novel coronavirus. In the case in question, the results confirmed the suspicion: both nose and throat swab samples from the patient came back positive. The 2019 novel coronavirus was officially in Canada.
***
China first reported the coronavirus to the World Health Organization (WHO) on New Year’s Eve, and despite the communist government’s effective quarantine of Wuhan—the city of 11 million people at the epicentre of the outbreak—the virus has spread to every continent except Antarctica. As of late February, mainland China has more than 78,000 confirmed cases, and more than 2,700 deaths. The virus has reached at least 55 countries and people have died of the infection in Iran, Italy, France, Japan, South Korea, Taiwan and the Philippines.
Cases that cannot be linked to a patient in China are cropping up around the world, in places as disparate as Iran and Italy. In Germany and the United States, there are now confirmed cases that have no known link to someone or somewhere with COVID-19, raising alarm bells that the virus could already be spreading locally.
READ: A made-in-Canada solution to the coronavirus outbreak?
Whatever chance there might have been to contain the virus, such that it was traceable to its origin point in Wuhan, seems to have passed.
Canadians, meanwhile, have repeatedly been told by government officials that the risk to the public remains low in this country. But that’s a bit misleading, says Michael Gardam, an infectious disease specialist and chief of staff at Toronto’s Humber River Hospital. Or, at least in light of COVID-19’s spread, short-sighted. “Let’s say you’re on the beach and you can see a tidal wave coming in the distance. It’s not here yet,” says Gardam. “At this very moment, the risk on the beach is low. But we know that’s soon going to change.”
Gardam’s message to the public would be more nuanced: the risk is low, but given recent outbreaks in Iran and Italy—which have caused the virus to spread across parts of Europe and the Middle East—it’s unlikely Canada will stay in this position for much longer.
And while the WHO won’t call COVID-19 a pandemic just yet, Gardam argues it would probably be best for Canada to consider it one. “We’re fooling ourselves if we think we’re going to stop this, so let’s shift our thinking to how we best slow down the spread,” he says. “By declaring a pandemic, it sends the message that if it’s not everywhere, it will be.”
Investors have already made that assumption. A sharp market downturn in late February was widely attributed to coronavirus fears, while biotech firms trying to develop a vaccine saw their stocks soar.
As anxiety rises across the globe, there are other practicalities to consider. If and when a wider outbreak reaches Canada, we can expect a surge of patients at emergency rooms, an increased demand for lab testing, and a need for more hospital beds. How prepared are we for the tidal wave of COVID-19?
***
Around the time Vanessa Allen’s lab confirmed that the Sunnybrook patient did indeed have COVID-19, Toronto Public Health officials were trying to contact those who had been in direct or indirect contact with the man.
“It’s an hour-by-hour account, detective work, to find out what sorts of activities they’ve been doing, where and with whom, since they’ve been ill,” explains Dr. Eileen de Villa, Toronto’s medical officer of health, offering a hypothetical example of the work her team does when any patient with an infectious disease is identified. “Where were you sitting on the plane? Did you go to the washroom? How much did you walk around? How did you get home from the airport? What did you do when you got home? Were people at your home when you arrived? Did you go to the grocery store to restock your fridge?”

Within hours of the first positive COVID-19 test result, a media press conference featuring politicians and representatives from Sunnybrook, Public Health Ontario and Toronto Public Health was convened. This type of transparency and communication from various health organizations has helped make Canada the second-least vulnerable nation in the world to outbreaks, based on the Infectious Disease Vulnerability Index (IDVI)—a 2016 research project created by the non-profit Rand Corporation in the aftermath of the Ebola and Zika virus outbreaks, which identifies countries most and least capable of handling outbreaks—trailing only Norway. And this position on the index is partly a reflection of the measures taken to improve preparedness in the wake of the 2003 SARS outbreak, which killed 44 people in Canada.
Back then, Sunnybrook had three members in its hospital infection control program, Leis says. Now they have 15. In 2003, the emergency department had one ventilation system, where air circulated throughout the entire department. Now, there are multiple zones with separate air circulation systems, and each zone has at least one negative-pressure room with its own circulation to the outside.
When there are suspected cases of an infectious disease, hospital staff have personal protective equipment at their disposal—masks, face shields, gloves—to protect them from virtually any high-consequence pathogen, “even the new ones that we don’t know about yet,” Leis says. Portable X-rays mean a patient doesn’t need to travel through the hospital for radiology. Even food trays for such patients are disposable, minimizing the need for staff to enter and exit the room.
The triage team keeps an active list of dangerous pathogens circulating in different parts of the world, allowing timely investigation based on a patient’s travel history. The list of countries of concern is updated daily.

All of this will stand Canada in good stead when patients do start coming to the hospital in greater numbers. The fact that China imposed large-scale quarantines—the “largest restrictions over the greatest number of people in the history of humankind,” says Isaac Bogoch, an infectious disease specialist at Toronto’s University Health Network—may also prove to be a mitigating factor. “That bought the world several weeks to prepare for widespread global transmission of this infection. Hopefully governments and health ministers used that time wisely.”
On Feb. 19, the daily number of new confirmed cases of COVID-19 globally dropped from thousands to hundreds. Meanwhile, the daily number of newly recovered patients was in the thousands. It might have appeared that the worst of the virus was behind us.
But then two people died in Iran that same day, the first fatalities in the Middle East. And then, on Feb. 20, more bad news: In what British Columbia’s provincial health officer called a “sentinel event,” a patient was diagnosed as Canada’s ninth person to contract the novel coronavirus. What made this case especially noteworthy is that the patient had never been to China. She had, however, recently returned from a trip to Iran.
***
On Valentine’s Day, a woman in her 30s boarded an Air Canada flight from Montreal to Vancouver. It was the final leg of her trip home after visiting family north of Tehran.
Somewhere on her long journey to Canada, she started to feel sick. A couple days later, her symptoms—fever, cough, headache and general fatigue—were serious enough to bring her to the emergency department. “She was concerned she might have been in contact with somebody who was sick,” says Bonnie Henry, B.C.’s provincial health officer.
The young woman figured it was probably the flu. The doctor who saw her did, too. There was no real reason to suspect COVID-19—the patient hadn’t been anywhere close to anyone who had travelled to China, let alone Wuhan. At least, not that she knew of. Iran didn’t even have a single confirmed case of COVID-19 at the time the patient first presented in emergency.
But because she had been travelling internationally, the doctor treating her figured it might be worthwhile to test for COVID-19—just in case.
When the test came back positive, Henry thought it must be a mistake. “I thought this could be MERS [Middle East Respiratory Syndrome] because it was circulating in that part of the world,” says Henry. But a MERS test came back negative.
“The clinician essentially had a hunch—so it was a bit of a fluke,” Henry says. “And we’re thankful, because it allowed us to contain this before it spread to too many people.”
Through the Public Health Agency of Canada, the case was reported to the WHO. Within days, Lebanon and the United Arab Emirates confirmed cases of COVID-19 in patients who had recently travelled to Iran. Soon, there were 43 confirmed cases in Iran, with eight deaths.
The numbers set off red flags with Ashleigh Tuite, an epidemiologist and adjunct lecturer at the University of Toronto’s Dalla Lana School of Public Health. For starters, China had reported a mortality rate of about two per cent, whereas almost 20 per cent of reported cases had been fatal in Iran. Not to mention, “with COVID-19, it normally takes a matter of weeks until someone dies,” Tuite says. “So if you’re seeing deaths reported, those people had been infected for presumably three weeks.”
Plus Iran has relatively little outbound air travel to Lebanon or Canada, at least not compared to countries like Iraq, Syria and Azerbaijan—which at the time had zero confirmed cases of COVID-19. The math didn’t add up.
Based on the virus’s dispersion from Iran to the U.A.E., Lebanon and Canada, Tuite and a handful of Toronto-based researchers crunched the numbers of Iran’s outgoing international airline travel volume in an effort to figure out the likely scale of the epidemic in Iran.
Their findings: Iran likely didn’t have tens of cases of COVID-19, as was officially reported. It probably had somewhere closer to 18,300.
Within days, the countries of Oman, Bahrain, Kuwait, Iraq and Afghanistan all had confirmed cases of COVID-19 stemming from people who had recently travelled to Iran.
And only a day after the Iranian deputy health minister coughed and sweated his way through a press conference denying claims his government was covering up the scale of the outbreak, he tested positive for COVID-19 and went into self-isolation.

***
Around the same time that a patient without any ties to China was diagnosed in Canada, the U.S. had a similar case in its sights—a person in California who hadn’t recently travelled or been exposed to someone with confirmed COVID-19. Although doctors considered the novel coronavirus to be a possible diagnosis for the Californian’s symptoms, they had to wait days for confirmation because of narrow criteria set by the U.S. federal agency responsible for administering tests. How far could COVID-19 have spread in that time? It’s tough to know for sure. The virus is thought to spread from person to person—be it via close contact or what are known as “respiratory droplets,” when someone coughs or sneezes. And its “R naught” rate—which estimates the number of healthy people a single contagious person would infect—is estimated to be between two and three, which is worse than the seasonal flu but not nearly as bad as measles. Meanwhile, symptoms like fever, cough and trouble breathing could take upwards of 14 days to appear.
As for how deadly it might become, a Chinese report from mid-February found the case-fatality rate of COVID-19 to be just over two per cent, which if accurate would put COVID-19 on par with the Spanish flu, the 1918 pandemic estimated to have killed at least 50 million people worldwide.
RELATED: ‘It felt like the end of the world’: From Wuhan to Canada in coronavirus quarantine
But experts have been skeptical of the data. To start, Chinese hospitals had been so overwhelmed with sick patients that it’s very plausible that many COVID-19 cases in the region went undetected, because their symptoms were so mild that people didn’t go to hospital. There are also questions about China’s transparency, particularly in light of the fact that Chinese officials initially tried to silence the doctor who had first warned his colleagues about the potential virus. (He died of the coronavirus weeks later.)
Without a better sense of the denominator—or the total number of COVID-19 cases, including the most mild—it’s tough to know the fatality rate.
What we do know is the daily increase in cases outside mainland China is now outpacing the number of cases within. And the death count is growing. In just over a week in late February, South Korea went from having 30 cases to 2,330, including 13 deaths. Seventeen more were dead in Italy, as of press time. Iran’s death count soon totalled 34. And strings of new cases have emerged in Singapore, Kuwait, Germany, Bahrain and Australia.
As soon as the first reports of the novel coronavirus started coming out of China, Isaac Bogoch knew it would only be a matter of time before the virus spread. That’s because, globally speaking, we’re still extremely vulnerable to outbreaks, Bogoch says, and a major reason why is the world’s growing interconnectedness via travel, tourism and trade. “Any person on earth can be at just about any other place on the planet in about 24 hours.”
To get a sense of how international travel could impact the spread of this coronavirus, Bogoch analyzed passenger loads and destinations from 10 major Chinese cities, using data from a three-month period in early 2019. He coupled that data with each country’s corresponding IDVI score.
Cambodia—a nation that receives hundreds of thousands of travellers from China, and also has a poor IDVI score—has only one confirmed case of coronavirus as of press time. Similarly, all of Africa, which does $200 billion worth of trade with China annually, has only three confirmed cases.
It’s unlikely these regions are simply lucky. “Some of these countries don’t have the capacity for case detection or case management,” Bogoch says. “And what happens over there can affect us here [in Canada]. We saw that with Ebola, chikungunya, Zika, SARS, MERS. It’s going to happen again.”
***
The world is not ready for this pandemic. At least not according to Canadian epidemiologist Bruce Aylward. Upon his return from a two-week mission to China on behalf of the WHO, Aylward commended the Chinese for their aggressive approach to containing and treating COVID-19 patients, while suggesting other countries equally prepare for larger-scale quarantines for people who come in contact with a person testing positive for COVID-19.
After the SARS crisis in 2003, the federal government equipped itself with sweeping powers in the event of a disease outbreak. The Quarantine Act, passed in 2005, allows Canada’s health minister to, among other things, divert travelling passengers or cargo, enforce mandatory medical screening and deem any place a “quarantine station” or “facility”—a private home, a hospital, a hotel, you name it. It allows for strict penalties, including fines up to $1 million and jail time, for people who fail to comply or who endanger others. This was the law that enabled the mandatory quarantine of those the Canadian government flew back from Wuhan.
Does the act allow for putting under quarantine places like a school, an apartment building, a city block, a neighbourhood, a town, a suburb or a city? “If the public health rationale is sufficiently strong, then yes, they could,” explains Steven Hoffman, a global health and law professor at York University and the scientific director of the Institute of Population and Public Health at the Canadian Institutes of Health Research. “The key being that it can’t just be this mass thing that’s limiting a whole lot of Canadians’ rights to liberty merely to contain a few people who are actually posing that risk.”
But a city-wide quarantine is inconceivable in the Canadian context, he says. Courts would likely find it unconstitutional. “It would likely be more in a precision way, focusing on individuals who are at risk of spreading something as opposed to the rather draconian mass quarantines that we would see in China,” Hoffman says.
If there is a surge of cases in Canada, public health authorities can be expected to start giving the kind of advice that’s helpful to prevent the flu. Wash your hands. Cough into your elbow. Stay home if you’re sick. “Public health authorities may encourage people to voluntarily reduce the number of mass gatherings,” says Hoffman, like work conferences.
With the number of cases surpassing 200 in Japan, in addition to the more than 700 cases on the Diamond Princess cruise ship off its coast, that country’s prime minister announced in late February that all schools would be shut for a month to help contain the virus’s spread. “Lots of studies show how few people we actually interact with on a daily basis,” says Hoffman. “Schools are where a lot of those different social networks intersect, such that it could be a place where spread could be enabled.”

As of late February, Hoffman would put school shutdowns in the category of “government overreaction.” But, he adds, “if a city in Canada faces a huge surge and it’s felt to be uncontrollable, you could imagine schools being temporarily closed,” he says, through government intervention. Still, it’s more likely that schools, workplaces or communities will ask for people to stay home voluntarily as the perceived risk of infection rises. “Some of the research shows that, when people are asked to self-quarantine, there are extremely high rates of compliance.”
Public health agencies have so far been focused on trying to keep people calm. But with stories emerging that suggest a wider spread of the virus is inevitable, public health officials will be at pains to assure people they have plenty of mitigation plans in place. “We do want the public to know we aren’t just sitting around waiting for new people to test positive,” says Chris Shewchuk, a spokesman for the B.C. health ministry. While trying not to prompt survivalist hauls from grocery stores, public health agencies will want people to consider how they might handle being asked to spend a couple of weeks at home riding out mild symptoms. Whether they can work from home. What it might mean for their loved ones or pets. “We’re not going to say, ‘go buy cases of water,’ ” Shewchuk says. “It’s very different from saying we need you to be able to, I don’t know, have enough canned beans.”
So far, patients in Canada with COVID-19 have voluntarily agreed to go into self-isolation at home, where local authorities can check in via phone to monitor them and ask them to check their own temperatures. But if cases become more severe—among elderly people with pre-existing heart or lung conditions who are most at risk, for example—that won’t always be an option.
And as the number of infections grow, the health care system needs protocols around how best to manage patients presenting with symptoms, and how best to treat those who test positive.
For Gardam, the biggest concern is that Canadian hospitals are routinely running over 100 per cent capacity, especially during flu season. “There is no room for extra people,” he says—not to mention that a significant portion of hospital beds are currently being used by elderly patients who do not need acute care, but aren’t well enough to go home. “It’s well-known we need tens of thousands of new nursing-home beds, and we’re not going to build those in three months,” he says.

To accommodate the influx, Humber River Hospital officials are already discussing the possibility of having to postpone elective surgeries by months, or even more than a year. Monthly check-ins might be delayed to every two months. Anything to open up another room, or another bed.
Then there are potential equipment shortages, where supply could be limited based on other countries facing similar outbreaks. “Most N95 respirators are made in China or the U.S.,” Gardam says. “We’ve stockpiled more than most countries, but if your stockpile runs out, you could have difficulty getting more equipment.”
And while plenty of hospitals have the resources to test for influenza, that’s not the case with COVID-19. “In Ontario, it’s basically all done at the Public Health Lab in downtown Toronto,” Gardam says. “If we start testing widely, that lab will be overwhelmed.”
With backlogs in testing and overcrowded hospital rooms, many people with mild symptoms might feel less compelled to get themselves checked out. “How many people in China or Italy have a sore throat and think: ‘I’m not going to the hospital. I might catch it in the waiting room’?” asks Gardam.
And there are still several unknowns, says epidemiologist Timothy Sly, including whether the virus can spread via the asymptomatic—meaning people who present no symptoms at all. “They could be on the bus, in the cinema or at school,” says the professor at the school of public health at Ryerson University. “And they could be spreading it around.”
Based on COVID-19’s transmission rates, one WHO adviser estimated two-thirds of the world’s population could get this virus. And even if the transmission rate is cut in half, that’s still roughly one-third of people getting infected.
As it stands, Gardam says it’s not overly dramatic to tell anyone they’re likely to get the coronavirus—even in Canada. “This is a new virus, so presumably none of us have any good immunity to it. With a lack of immunity, why wouldn’t we get it?” he asks. “The odds are good that I’m going to catch this. The odds are good that you’re going to catch this. And chances are we’ll be fine.” In fact, a huge chunk of the population might not even realize they get it.
But then there’s that very small percentage of the population, mostly the elderly, who won’t be fine. If COVID-19 spreads across Canada, infecting half the population, and the virus has a mortality rate of even a fraction of one per cent, tens of thousands of Canadians would die.
“If you think back to what happened during the Spanish flu, every person had a story of a family member who died,” Gardam says. “It’s possible we could be getting into that scenario.”
This article appears in print in the April 2020 issue of Maclean’s magazine with the headline, “A planet infected.” Subscribe to the monthly print magazine here.