Doctors want the right to pull the plug
The battle between doctors and patients’ families over end-of-life care has just begun
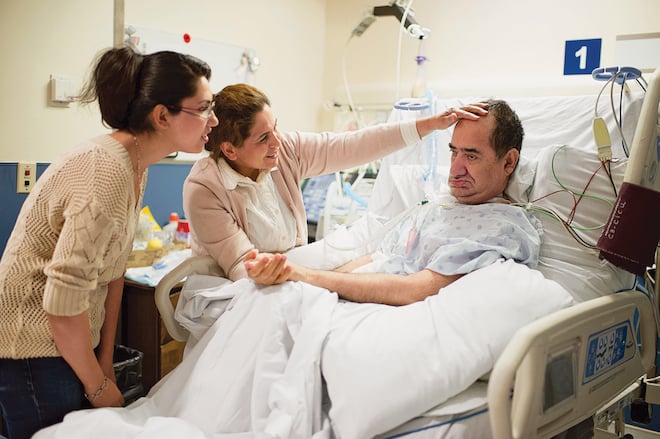
Photo illustration by Andrew Tolson / Levi Nicholson
Share

On the morning of Oct. 18, Mojgan Rasouli and her mother, Parichehr Salasel, left their home in Toronto’s north end and boarded the subway for downtown. This was a day they’d anticipated for years, yet Rasouli, a self-possessed 30-year-old, felt calm.
Approaching the offices of their lawyer, Gary Hodder, they took note of the news vans parked outside. About half an hour before, the Supreme Court of Canada had announced its ruling in a case that will have life-and-death implications for every Canadian—and, most immediately, for Mojgan’s father and Salasel’s husband, Hassan Rasouli. As the two women rode the elevator to the 22nd floor, the Supreme Court decision was already dominating headlines. Yet Rasouli and Salasel still had no idea which way the verdict had gone.
In 2010, Hassan Rasouli, an Iranian engineer, emigrated to Canada with his wife and two children (Mojgan’s brother, Mehran, is 26). That October, he underwent surgery at Toronto’s Sunnybrook Health Sciences Centre to have a benign brain tumour removed and contracted an infection that left him profoundly brain-damaged. For the last three years, the 61-year-old has been kept alive by a mechanical respirator inserted into his trachea; he’s fed and hydrated through another tube, in his stomach. His doctors, who say Rasouli will not recover, wanted to “unplug” him. His family said no. Devout Shia Muslims, they believe that every human life is sacred, and they’re convinced that Hassan’s health could improve. Salasel, a physician in Iran, is at her husband’s bedside daily, and reports that he shows signs of consciousness, like giving the thumbs-up, or opening his mouth and sticking out his tongue on command. In a five-to-two ruling, the Supreme Court sided with the Rasoulis. When mother and daughter stepped off the elevator into Hodder’s office, and learned the result, cries of joy echoed down the hall.
- RELATED: Right To Die: Why Quebec will likely become the first province to legalize assisted suicide
Death is the stark reality of life. Yet, with the tools of modern medicine, we can now postpone it for a startlingly long time. In the case of patients such as Rasouli, who can no longer speak for themselves, some family members insist that everything medically possible be done to keep them alive. Doctors argue that aggressive interventions can prolong a patient’s suffering—that this puts the doctors themselves in an untenable ethical position. They want the right to decide when it’s time to end life support, and let the patient die. “Physicians often feel like torturers,” says Arthur Schafer, director of the Centre for Professional and Applied Ethics at the University of Manitoba. Patients who can’t swallow must have fluid suctioned from their lungs. “It’s like having a hot poker put down your throat. Bedsores are inevitable. They get infected, and must be surgically scraped.”
The Supreme Court ruling does little to bring closure to this debate. On the contrary, it’s expected to embolden more families to challenge physicians over end-of-life care. Given Canada’s aging population, and advances in medical technology, the battle between doctors, patients and their families over whether or not to “pull the plug” is only beginning. It’s still rare for doctors and patients, or their substitute decision-makers, to disagree over end-of-life care, but it’s happening more often. Ontario’s Consent and Capacity Board, an independent tribunal created 17 years ago to deal with such situations, has heard a number of gut-wrenching cases dealing with the elderly, the infirm, even babies. Since 2009 there’s been a “dramatic increase” in the use of the board to resolve end-of-life cases, according to a 2013 study in the Journal of Critical Care.
In attempting to stop Rasouli’s life support, his doctors didn’t go to the Consent and Capacity Board—they skipped that step. Drs. Brian Cuthbertson and Gordon Rubenfeld, intensive-care physicians at Sunnybrook, have argued that they don’t need a patient’s consent (or that of his substitute decision-maker, in this case, his wife, Salasel) to end a treatment that has no medical benefit, as they see it, and may even be causing the patient harm. The Supreme Court disagreed and said they should have gone to the board. So now, Ontario’s Consent and Capacity Board has the seal of approval of the highest court in the land. And the Rasouli family’s legal battle may not be over. If the doctors wish, they can now take the case to the Consent and Capacity Board, which could step in and have Hassan Rasouli taken off life support, once and for all.
Despite this possibility, Mojgan Rasouli was composed after the Supreme Court ruling. “Any other decision would have surprised me,” she says. “Nobody can draw a line for the end of life. Not even doctors.”
In July 2007, the Consent and Capacity Board heard the case of a patient identified as “Mr. C.D.” He was an 81-year-old man from St. Catharines, Ont., and a Second World War veteran who’d come to Canada “with nothing,” as his family explained, working hard to become a successful businessman. He was suffering from dementia and was being fed through a tube into his stomach. He had bedsores and infections his body could no longer heal. Mr. C.D.’s doctor believed her patient should be taken off life support and put on palliative care. It would hasten his death, she said, but give him a better quality of life at the end. His wife adamantly disagreed, refusing to consent.
As Mr. C.D. could no longer speak for himself, Mrs. M.D. was his “substitute decision-maker,” a legal term defining who can give consent to medical treatment when the patient himself cannot. Both were devout members of the Greek Orthodox Church. Mrs. M.D. testified that her husband was a “fighter,” and would wish to stay alive for as long as possible. (This was his daily philosophy, she said, although the two had never discussed life support.) Mrs. M.D. even refused the doctor’s requests to increase her husband’s pain medication, worrying it would render him unconscious and unable to recognize her and their daughters. When Mr. C.D.’s family members visited him, they believed they could still detect “joy in his eyes.”
In the past decade, Ontario’s Consent and Capacity Board has heard about 25 such cases, “more than all the courts in the country combined,” according to Mark Handelman, a Toronto health-law lawyer, who has served as its vice-chair and senior lawyer member. (Only the Yukon has a similar system, called the Capability and Consent Board.) The Consent and Capacity Board has about 150 appointed members, one-third of them psychiatrists, another third lawyers and the rest laypeople, says Handelman, who served there for a decade. Hearings are held by three-person panels as close as possible to where the patient is being treated, within a week of the initial application. Decisions are rendered within one day.
In the case of Mr. C.D., the board ruled with his doctor. The written decision acknowledges his wish never to give up the fight. “But, he did not. He fought dementia for as long as humanly possible, perhaps longer than humanely possible.” It directed Mrs. M.D. to: consent to removing her husband’s nutrition and hydration; boost his pain medication; and start palliative care. The board’s decision does not state whether Mrs. M.D. complied, but in cases where substitute decision-makers don’t consent following a ruling, they are no longer considered fit for the role. (Parties can appeal to the Superior Court of Justice.)
In January 2011, when Hassan Rasouli’s doctors found themselves at loggerheads with Salasel, they decided not to go to the Consent and Capacity Board. In an active challenge to the way these cases are handled, they said they would unplug him unless Salasel got a court order to stop them. She and her children, who’d been in Canada mere months at this point, were at a loss. They found Hodder, their lawyer, through a friend in Toronto’s expatriate Iranian community. After two lower courts stopped doctors from unilaterally withdrawing life support without Salasel’s consent, the Supreme Court weighed in.
It found that ending life support does in fact constitute a “treatment” that requires consent: It has the “health-related purpose” of preventing a patient’s suffering and indignity; it can entail “physical interference” with the patient’s body; and it’s closely tied to palliative care, which clearly requires consent. As Chief Justice Beverley McLachlin wrote in the ruling: “By removing medical services that are keeping a patient alive, withdrawal of life support impacts patient autonomy in the most fundamental way.” The chief justice also noted that Ontario’s Consent and Capacity Board has handled these cases for many years, and that they shouldn’t be sent back to the courts. Given the ruling, Handelman believes we could start seeing similar tribunals pop up across Canada.
Schafer, the ethicist at the University of Manitoba, calls the Supreme Court decision “disappointing, muddled and incoherent.” With this ruling, “the right to refuse treatment becomes the right to demand treatment,” he says, even when doctors feel it’s pointless or harmful to the patient. (The two dissenting justices felt these end-of-life cases should be decided by the courts, not by the Consent and Capacity Board.) The verdict touches upon doctors’ ethical dilemmas in these cases, yet it does little to soothe them. In 2008, three doctors resigned from a Winnipeg hospital rather than continue to treat Samuel Golubchuk, an elderly patient with minimal brain function. Doctors wanted to remove Golubchuk from life support; his family sought a court order to stop them, believing this would violate his beliefs as an Orthodox Jew. (Golubchuk died after almost eight months on life support, and the family later dropped its lawsuit against the hospital.)
The Supreme Court also didn’t address one of the most pressing issues in our health care system. To treat just one patient in a bed in the intensive care unit (ICU) costs an estimated $1 million per year. The Sunnybrook doctors, however, chose not to raise this in their legal battle. “Physicians don’t make decisions for patients based on resource allocation issues,” says their lawyer, Erica Baron of McCarthy Tétrault. In the Rasouli case, “it wasn’t factored into the decision-making.” Even so, it’s a reality Canadians must consider. As Handelman notes, “It comes down to: Are we going to keep your grandfather alive in a vegetative state in an ICU bed that I need for three days after bypass surgery?”
Cutting-edge research is making the line between life and death ever blurrier. After falling into a coma, Rasouli was diagnosed as being in a persistent vegetative state, meaning he was completely unconscious and unaware. Yet, in 2012, his diagnosis was upgraded slightly, to “minimally conscious.” The work of Adrian Owen, a neuroscientist at the University of Western Ontario, suggests that some vegetative patients show signs of consciousness when their brains are scanned—and that a few can even answer questions by modulating brain activity. Rasouli’s family are certain he is awake, despite what the doctors say. “I see from his eyes, he understands everything that happens around him, but cannot respond,” Salasel says.
“As lawyer to this man, this is something that’s haunted me,” Hodder says. “He may be lying there in his hospital bed, listening to people talk about him. He may be completely aware. Medical science doesn’t always get it right,” the lawyer adds and, for that reason, “decisions are not exclusively the province of [doctors].”
The legal floodgates are opening as more newly empowered patients and their families fight for a say in treatment. Joy Wawrzyniak, a nurse in Oshawa, Ont., filed a lawsuit against Sunnybrook and two of its doctors, Donald Livingstone and Martin Chapman, over the 2008 death of her father. Douglas DeGuerre, then 88, was a Second World War veteran living in the hospital’s K Wing, a care facility for vets. On Sept. 17, DeGuerre had both legs amputated above the knee. Before the surgery, Wawrzyniak—her father’s substitute decision-maker—told the doctor that if her father went into cardiac arrest, they should do everything possible to revive him. DeGuerre got through the surgery and was sent to the ICU. Wawrzyniak’s statement of claim alleges that, although she instructed several times that her father was to be treated as “full code,” meaning all life-saving measures be taken, doctors changed his status to “do not resuscitate,” unbeknownst to her. On Sept. 22, she came to the hospital to visit her father and found him struggling to breathe. DeGuerre went into respiratory arrest and died.
Now that the Supreme Court ruling has come, Wawrzyniak’s lawyer, Barry Swadron, says, “We intend to move forward very quickly. Whenever there’s a disagreement between the family and doctors, they have to go to the Consent and Capacity Board. Joy didn’t have that opportunity.” Lawyer Daphne Jarvis, who’s representing Sunnybrook, says this recent ruling won’t have an impact on the Wawrzyniak lawsuit. “The Court decided only that withdrawal of life support in a situation like Mr. Rasouli’s constitutes treatment for which consent is required,” she wrote in an email. “The DeGuerre case is totally different. It remains the case that medical judgment determines whether a treatment such as CPR is to be offered.” The doctors’ legal team would not comment.
Sunnybrook has earned a reputation as a hotbed for physician-activists. “The Rasouli case is not unique out of Sunnybrook,” says Handelman, who’s been involved in a handful of other disputes there. But Dr. Andy Smith, executive vice-president and chief medical executive, says any perception that Sunnybrook doctors are aggressively taking aim at end-of-life laws is simply a matter of sample size. With around 90 ICU beds, Sunnybrook has the biggest ICU in Canada, he says. “Over 4,000 people each year come in as new admissions to these high-end critical-care beds,” Smith notes. “This is not a Sunnybrook-specific issue. It’s arising across the country, all the time.”
And not just over the elderly. One case heard by the Consent and Capacity Board in September 2007 concerned a patient identified as “EJG,” an eight-month-old baby who suffered oxygen deprivation before birth, leaving him in a vegetative state. He didn’t respond to pain, sound or discomfort. He couldn’t eat or drink and was fed through a tube. His eyes could not blink and needed special ointment to keep them from drying out. He was the size of a child of 2½ months. While this baby might survive many years, kept alive by increasingly invasive medical procedures, he would not improve. EJG’s doctors wanted to wean him from the ventilator; if he could not survive, they proposed letting him die, supporting him with comfort care. The baby’s parents wouldn’t consent, saying that God would heal their son, or that medical science would one day find a cure. The board sided with the doctor.
Handelman hopes the Rasouli verdict will convince more people to discuss their end-of-life wishes. “You sometimes have family members who believe they’re doing the right thing by fighting to keep a loved one alive,” he says, “when the loved one would not have wanted it.” As for Rasouli, it’s impossible to say at this point whether he wishes to live in such a state. His daughter, who describes him as a creative, charming and ambitious man, with a lively sense of humour and a love of Persian music, says the Muslim faith is the foundation of their family. “Our religious beliefs are very personal,” she says. “The life of the human is precious.”
After an emotional press conference at Hodder’s office, wife and daughter went to visit Hassan Rasouli, as they do each day. “In the evening, my mother-in-law, my husband and our friends all came to the hospital,” says Mojgan Rasouli, who was married earlier this year. That day, she told her father of the Supreme Court verdict. She squeezed her father’s hands. She says “his eyes were very bright.”