D.I.Y. DNA: Genetic testing at home is risky business
What harm could come from sending off a sample of your DNA to find out your genetic history and potential health problems?
Share
Update: On May 4, 2017, Bill S-201, the federal Genetic Non-Discrimination Act, was passed into law
On a midweek morning in 2015, Tim Cottee clicked shut his office door, woke his computer and girded himself for a piece of life-changing news. Weeks earlier, the 42-year-old executive at a Winnipeg financial services company had signed up with 23andMe, a California-based company that provides DNA testing and health information to Canadians over the web. His results were now in—Cottee’s iPhone had chimed when the notification landed—and he was feeling a mix of excitement and dread: Six years ago, his mother had died at 69 of Alzheimer’s disease, and these results would reveal whether Cottee was carrying a mutation of the APOE gene known as the e4 variant, the strongest hereditary risk factor for Alzheimer’s.
“Obviously, my mom had some kind of predisposition,” Cottee had told Maclean’s a few days before receiving the report. “When you go and visit your parent in a care home—when they’re the only resident there in their 60s while everybody else is on the far end of their 70s or older—that tells you something.”
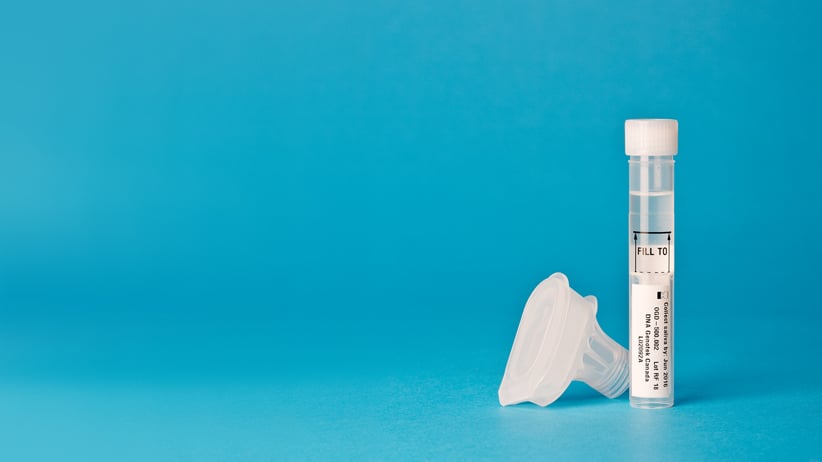
Cottee is not the first person to suspect a Trojan horse is lurking in his DNA. The atavistic fear of flaws in our biological coding is an inescapable feature of the genetic era, going back to the mapping of the human genome in 2003. What’s changed is the ease with which we can put those misgivings to the test. Cottee is one of about 20,000 in this country who have swallowed hard and clicked on their 23andMe health results since the firm took advantage of a gap in Canadian laws five months ago and began offering its health profiles to members living north of the border. For $199, the company couriers its members a “collection kit”—essentially, a test tube into which you spit—which goes back to the company’s laboratories in the U.S. for genotyping. Within weeks, members can log on to the company’s website to view a raft of information ranging from the amusing (are you predisposed to hate cilantro?) to the soul-crushing (are you predisposed to Parkinson’s disease?).
Not everyone is psychologically prepared—especially those who had been tested so they could trace their geneaology, the other arm of 23andMe’s thriving online enterprise. “I had a bit of a cry,” said Candace, a 47-year-old mother of two from Brantford, Ont., who learned she has one copy of the e4 variant (she asked that her identity be withheld). “It’s like, whoa, I didn’t know this was in me. Oh my god, what if I pass it on? It’s very jarring, at first.” So weighty are the findings, and so challenging to place in proper perspective, that in November 2013, the U.S. Food and Drug Administration sent a letter to 23andMe asking it to stop providing health results to its American members. The service amounts to a medical diagnostic device that the FDA had not yet approved for marketing, the letter said. 23andMe quickly complied.

The company has faced no such roadblock in Canada. Here, direct-to-consumer DNA testing has fallen through the yawning chasm known as the constitutional division of powers. Health Canada says the service falls under the jurisdiction of the provinces, while the provinces show little interest in regulating testing that is done outside their borders (a spokesman for the Ontario ministry of health said they don’t consider it their jurisdiction). No surprise, then, that 23andMe has ramped up efforts to market its genetic health service north of the border since the FDA clipped its wings. Canada, in the meantime, remains the only G8 country without some sort of law governing how genetic test results can be used by insurers and employers, despite warnings that people who receive bad news could face discrimination when they try to obtain coverage or get jobs.
All of which suggests the country is no more ready for the new era of genetic health testing than the thousands of Canadians on whom 23andMe has been dropping eye-opening and, in some cases, heartbreaking information. “This is being marketed as a fun thing to do,” says Bev Heim-Myers, chair of the Canadian Coalition For Genetic Fairness, an organization advocating for legislation banning discrimination based on genetic test results. “But it can go from fun to devastating. This information can then be shared and used against the person. Until we have laws protecting genetic information, this is a dangerous thing.”
We can’t say we weren’t warned. Long before the Human Genome Project charted almost all of the three billion base pairs of human DNA, ethicists and futurists sounded alarms about the potential misuse of genetic information, as testing became cheaper and more widely available. The term “genoism”—unethical discrimination based on genetics—was coined by Andrew Niccol, director of Gattaca, a 1997 movie that portrayed a society driven by eugenics rather than merit. The film’s foresight, alas, proved greater than its cultural impact. Canada, for one, has been drifting for years toward the world it depicted.
The plunging price and ready availability of genetic testing is a key part of that new reality. The price to fully sequence all three billion base pairs has been driven down to about $2,000, from the billions spent on the Human Genome Project. But the real game-changer has been Anne Wojcicki, the wife of Google billionaire Sergey Brin (the two are now separated), who realized the true value of genetic testing lay in aggregated data that could, in turn, be sold for medical research and development. In 2006, she founded 23andMe with her partner, Susan Avery, naming the company after the 23 pairs of chromosomes in a human cell. The following year, they began offering $999 genotyping—a process that identifies about 750,000 of the genome’s DNA base pairs. By late 2012, the firm was offering $99 tests to its American members, while asking them for consent to share their genetic data, stripped of identifying personal information and lumped in with hundreds of thousands of others’, for the purposes of medical and pharmaceutical research.
The company has since shared that information with partners ranging from pharmaceutical giant Pfizer and the U.S. National Institutes of Health, to advance research into everything from obesity to Parkinson’s disease. (Wojcicki took a special interest in Parkinson’s after 23andMe testing revealed in 2008 that Brin carries a gene mutation linked to the disease.) In 2015, the firm announced it is launching its own research division to develop drug therapies.
The company’s growth is part of a gold rush occurring at the nexus of big data and Big Pharma, with Silicon Valley players such as Apple developing apps that encourage customers to self-report personal health information in the name of advancing medical research. And it’s not as though 23andMe, which is financially backed by Google, keeps its real line of business a secret. The firm notifies its members about every new collaboration, while encouraging them to participate in online surveys about their traits, tastes and histories. (A recent one asks them to render judgment on the colour of that blue-or-gold dress that went viral on the web.) The customers, meanwhile, receive a downloadable file containing their raw DNA data, which they are free to share with doctors or genetic counsellors, along with a report of 110 traits, inherited conditions, drug responses and genetic health risk factors.

Reading the report can be a strangely out-of-body experience—like learning secrets about a friend you thought you knew well. This writer has gene variants linked to high susceptibility to the norovirus (a.k.a. the “winter vomiting bug”), as well as the ability to metabolize caffeine quickly (gratifying, given current consumption patterns).
Of greater concern to genetic experts, though, are the heavyweight indicators such as those for Alzheimer’s, breast cancer and Parkinson’s. Before disclosing them, the 23andMe site requires members to open a printed primer explaining the results and their limitations. In the case of the Alzheimer’s APOE variants, they can also watch a video presentation by a Harvard Medical School doctor, Robert Green, who assures members he’s not being paid for his appearance. “Finding you are at somewhat higher risk might cause distress,” Green acknowledges in the clip. “So give it some thought. If you think this information might distress you, you can simply decide not to view it. Or feel free to discuss it with a doctor or a genetic counsellor before you unlock and view your results.”
Such notes of caution litter the site. But critics complain they aren’t enough, because the thought of revelatory news a couple of clicks away is too tempting for most people to pass up. Adverse findings can trigger panic, while an absence of indicators provides false reassurance, warns Allie Janson Hazell, president-elect of the Canadian Association of Genetic Counsellors. Furthermore, putting the information in perspective requires expert understanding of the limitations of a genetic test, as well as a person’s family history, she says. Janson Hazell points to 23andMe’s tests for three mutations associated with breast cancer, which are most prevalent in people of Ashkenazi Jewish descent. “If I, a person of non-Ashkenazi ancestry, get a normal result back, I might feel reassured, even if there’s lots of breast cancer in my family,” she says. “This is where the potential for harm comes in.”
As you might expect, what is framed in Canada as “potential for harm” takes the form of direct accusation in the United States. Less than a month after the FDA fired off its warning letter to 23andMe, the company was fending off a class-action lawsuit alleging that its health reports were scientifically meaningless marketing tools allowing it to build up its inventory of saleable gene data. One commentator on Forbes.com warned that quality control is an issue at 23andMe, accusing the company of extrapolating from “a few reports about specific populations.”
Emily Drabant Conley, 23andMe’s director of business development, brushes aside the knocks, saying the company strives to strike a balance, presenting scientifically accurate information in a way that non-experts can understand. “We’re seeing with our customers that they do understand the information, and they do find it relevant,” she says from 23andMe’s offices in Mountain View, Calif. At the root of the model, she adds, is an individual’s right to obtain information about himself so he can make healthy adjustments to his lifestyle. “There are many cases where this information really changes the trajectory of someone’s health,” says Drabant Conley, who has a doctorate in neuroscience. “He or she can find out a piece of information he or she didn’t know, that you could really only ascertain through genetics.”
Company officials are also quick to note that the FDA recently eased its stance on 23andMe’s marketing, allowing it to advise customers whether they have markers for Bloom’s syndrome, a rare condition associated with short stature, sun sensitivity and increased cancer risk.
Whatever the criticisms, direct-to-consumer DNA test results appear to be good enough for the insurance industry. Five years ago, knowing that many Canadians would soon be able to afford the tests, the association representing the country’s life and health insurers issued a statement claiming the right to ask applicants if they’d had genetic testing done. If so, they’d ask for the information before agreeing to a policy, they said, just as they would demand disclosure of other medical records.
The point, says Frank Zinatelli, vice-president of the Canadian Life and Health Insurance Association, was to ensure equal footing between insurer and client: Insurers don’t demand genetic testing from anybody who hasn’t already had it done, he stresses; nor can they reopen existing policies based on newly discovered adverse results. But people who knew they had genetic indicators for degenerative diseases like Huntington’s could conceivably rush out to buy policies, Zinatelli argues, upsetting actuarial calculations and ultimately costing everyone. “Let’s remember the definition of insurance,” he says. “It is financial protection against unanticipated loss” [emphasis his].
Maybe. But that hasn’t stopped critics from citing the insurers’ position as proof that Canada is hurtling toward a Gattaca-like society, where the genetically flawed live diminished lives, cut off from important opportunities or benefits. In 2009, researchers at the University of British Columbia published a survey in which 40 per cent of 233 people with family histories of Huntington’s disease reported they’d experienced some sort of discrimination based on their risk of developing the devastating hereditary brain disorder—especially when it came to getting insurance. Fully 29 per cent said insurers had rejected them, increased premiums or asked them to take genetic tests. (The highly predictive Huntington’s mutation, it should be noted, is not part of 23andMe’s health results package.)
And doctors warn that fears of discrimination are discouraging people from obtaining genetic tests that could head off life-threatening diseases. At a Senate committee hearing last fall, Dr. Ronald Cohn, chief of clinical and metabolic genetics at Toronto’s Hospital for Sick Children, told the story of a 12-year-old girl whose parents delayed getting her tested for a hereditary connective-tissue disorder because of concerns about the entire family’s insurability if the results became known. The girl could have one of two conditions, Cohn said, for which the treatments are vastly different. Without the test, “I can’t manage the child’s care,” he added. “I have her come back frequently for echocardiograms to make sure everything is in place, until the family moves forward and I know which disease I’m going to deal with.”
Disturbing as their anecdotes are, advocates such as Cohn and Bev Heim-Myers have had a hard time getting attention on Parliament Hill. In 2013, James Cowan, a Liberal senator from Nova Scotia, tabled a private member’s bill in the upper chamber prohibiting anyone from demanding a genetic test, or the results of a genetic test, as a condition of providing goods or services. Bill S-201 would have amended the Canadian Labour Code to stop employers from requiring workers to take or disclose the results of genetic tests, while adding genetic characteristics to the Canadian Human Rights Act as a prohibited ground of discrimination. It carried the power of criminal law, with fines as high as $1 million and prison terms as long as five years.
23andMe counted among the bill’s most enthusiastic supporters. But the law’s key provisions were voted down in February [2015] by the Conservative majority in the Senate—in part because the Harper government promised in its 2013 Throne Speech its own legislation against genetic discrimination. A spokeswoman for Justice Minister Peter MacKay said in an email last week that the government still intends to act on the file, but she did not specify when. And the fear factor is running high. When Cohn and the staff at Sick Kids recently offered free full-genome sequencing to 330 children in care at the hospital as part of a study, more than 100 of the families refused, citing concern about genetic discrimination.
Curiously, few of 23andMe’s Canadian members seem to share those qualms. Several contacted over the past few weeks told Maclean’s they welcomed the health results, and some bristled at the idea of government interference in the service. “I’m fine with the Canadian lack of regulation here,” said Davis Simpson, a 45-year-old Calgarian who signed up to do geneaological searches and regards the health findings provided later as a bonus. “I strongly oppose any action to deny me access to my own health information.”
Most, including Simpson, saw the need for some control of genetic discrimination, but they tended to view the issue mostly as a matter of personal choice. “No one has a right to my body, with or without my explicit consent,” said Nancy, a member from Minden, Ont., who asked that her identity be withheld. “Logically, that includes my personal genome.”

Still, even savvy users like Cottee admit that opening the results unleashes a flood of unforeseen implications, raising as many questions as it answers. After drawing a breath and clicking through to his APOE findings, Cottee was stunned to find that he carried neither copy of the e4 variant. He then took his raw data and loaded it onto a website that screens it for 15 other, less reliable genetic mutations connected to Alzheimer’s. Again, nothing.
“It was a weird thing, because I didn’t actually feel the sense of relief I thought I was going to,” Cottee recalls. “I’d had this feeling of inevitability all along. So why wasn’t I feeling more positive?” It was then that the limitations—or was it the value?—of his tests hit home. Alzheimer’s is a multi-factoral disease, he knew, linked to everything from genetic mutations to obesity. If, for example, his mother never had the APOE gene, then something else had made her vulnerable to Alzheimer’s. She was overweight, and her unhealthy lifestyle had led to diabetes, he notes. But Cottee has already taken steps to avoid those risk factors, which leaves him in the same boat as the rest of us at the onset of the genetic era: awash in information, yet woefully short on certainty—and a little afraid of what he might learn next.
Update